Mitochondrial disease: the genomics challenge
Mitochondrial diseases are overwhelmingly genetic in origin, so why are gene therapies so difficult to develop? We take a deep dive to find out more.
Genome editing plays a vital role in our ability to understand and treat rare diseases. However, when disease-causing variants occur in the mitochondria, we are still largely in the dark. But why are mitochondrial conditions such a unique case, and what makes them so difficult to study?
Mitochondrial disease
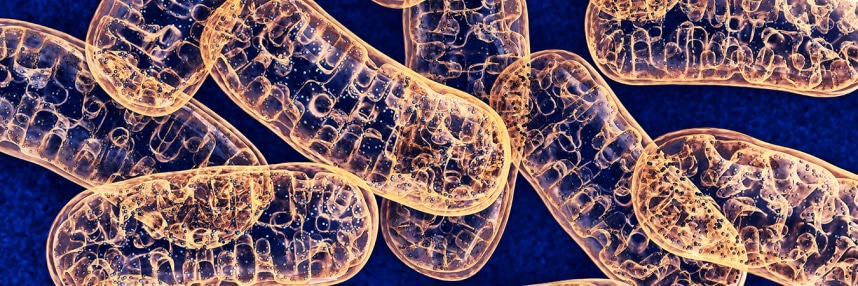
Mitochondria are organelles – self-contained pieces of cellular machinery located in the cytoplasm of almost every cell in the human body. They are the site of the series of chemical reactions that generate energy to power the cell’s functions, and so are found in greater numbers in cell types that need a lot of energy, such as muscle.
A quirk of evolutionary history means that mitochondria have their own genome – a circular piece of DNA containing just 37 genes, entirely distinct from the chromosomal genome found in the cell nucleus.
Mutations in these genes can cause mitochondrial diseases, which can vary in severity, often depending on what proportion of a person’s mitochondria are affected. These conditions are rare but collectively affect between 1-in-4,000 and 1-in-6,000 people, and are often life-limiting. Some mitochondrial disorders can also be caused by mutations in the nuclear genome.
Treatment and research
No curative therapies are available: current treatment options can only address symptoms, and not the cause of the problem.
Mitochondrial donation is permitted in the UK for families affected by mitochondrial disease, but this aims to prevent the disease being passed on to the next generation, and cannot treat people who are already affected.
So, what about people who have already been born? The difficulty is that research into the mitochondrial genome is years behind that of the genes in the nucleus; there has never been a way to change the mitochondrial DNA without destroying the mitochondria, which has slowed down research and the development of treatments.
The limitations of CRISPR
One of the cornerstones of genetic research is being able to reproduce human mutations in animal models – often mice. Modern approaches to genome editing, especially CRISPR-based methods, have made doing this much easier for many conditions, but not for mitochondrial disorders.
Each mitochondrion is encased in its own membrane and we have discovered that RNA molecules are not transported through it. CRISPR-Cas9 genome editing depends on a guide RNA which binds to the target DNA sequence and allows the Cas enzyme to cut.
Additionally, the CRISPR-Cas9 genome editing approach relies on the cell’s own DNA repair mechanisms to re-join the cut ends after the edit is made. The mechanisms through which this takes place in the nucleus do not appear to be present in the mitochondria.
A potential treatment
A recently-published Nature paper has demonstrated a new approach that has made it possible to precisely edit the mitochondrial genomes of human cells in vitro for the first time.
The approach combines features of CRISPR and base editing as well as TALENS – a genome editing technique that preceded CRISPR. It allows a cytosine base (one of the four DNA ‘letters’) to be converted to a thiamine, and so has the potential to correct some point mutations in the mitochondrial genome.
There will be many more hurdles to overcome before effective gene therapies can be developed, but recent research is indicating a positive future outcome for those affected by mitochondrial conditions.
–