4.50 from Paddington to Genomics
A look at the journey from arsenic and ancient alchemy to modern-day pharmacogenomics
In her 1957 novel 4.50 from Paddington, Agatha Christie’s Dr Quimper, in the knowledge that “people don’t all react alike to poisons”, murders Alfred Crackenthorpe with arsenic. As he explains: “Gastric cases vary, of course, but there were certain indications that would have been, shall we say, more consistent with arsenical poisoning than with plain gastro enteritis. Mind you, the two things are very much alike. Better men than myself have failed to recognise arsenical poisoning – and have given a certificate in all good faith.”
As Paracelsus once remarked: “The right dose differentiates a poison and a remedy.” And this is a fact that all clinicians, and oncologists in particular, are well and increasingly aware of, writes Alain Li Wan Po.
A careful balancing act
Quimber was not the first to use arsenic for poisoning; the Borgias made it into an art – and arsenic murders continue to be reported worldwide.
With its roots in alchemy, drug therapy continues to include medicines that have been used empirically for thousands of years. Arsenic is a constituent of several Ayurvedic medications that still lead to case-reports of chronic poisoning. Yet arsenic has over recent years emerged as one of the few medications that can cure cancer, and one cancer in particular: acute promyelocytic leukaemia (APL).
With the help of genomics and molecular investigations, the mechanisms for the extraordinary effectiveness of this ancient medication, once reported on by Conan Doyle in the Lancet of 1882 (before his greater fame as the Sherlock Holmes story-teller) is becoming clearer. Although Doyle reported some success for his one leukemic patient, the then leading French Textbook of Medicine was muted in its appraisal, saying that “arsenical therapy gave without doubt the least bad results” among therapies available. Within two decades, Paul Ehrlich would introduce his arsenical compound 606 as the first truly effective drug against syphilis.
Validation of the use of arsenic in APL treatment had to wait for another century until little known but innovative investigators from China brought attention to their impressive results. Today, therapy based on all-trans retinoic acid (ATRA, also called retinoid) and arsenic trioxide (ATO) is regarded as the new standard of care for most APL patients.
Differentiation therapy and molecular mechanisms
The discovery of the efficacy of retinoid and arsenic in APL arose from a search for compounds that might induce the terminal specialisation (differentiation) of cancer cells. The rationale is based on the fact that cancer cells are proliferative, whereas fully specialised, mature cells lose this ability in their final, differentiated state. This approach to cancer treatment became known as differentiation therapy, in contrast to conventional chemotherapy that aims to kill the cancer cells directly. Among the first generation differentiation agents were cis-retinoic acid and racemic retinoic acid which contains both cis and trans isomers (variants of retinoic acid with the same molecular structure but differing in their three dimensional arrangements), and 5-azacytidine.
Unlike cis-retinoic acid, ATRA is highly effective even in patients who are non-responsive or resistant to chemotherapy. However, in the first 1988 report, a third of the complete responders (CR) had relapsed within 5 months, even when maintained on chemotherapy. The authors concluded that “a method of maintaining and prolonging the duration of CR” was required. This method came in the form of combination therapy with ATRA and ATO; researchers reported in 2009 that of 85 newly diagnosed APL patients treated with the combination, the 5-year relapse-free survival was 95%. Equally impressive results were reported in a 2013 Italian trial, albeit with a shorter follow-up.
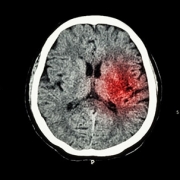
The genetic mutation that causes APL is a reciprocal exchange (translocation) of bits of chromosomes 15 and 17, leading to the formation of an abnormal protein that inhibits the normal differentiation of precursor cells to mature, functional white blood cells. Unless treated, the immature cells literally clog the blood vessels of the patient, causing massive, rapidly life-threatening bleeding.
APL is not the only leukaemia associated with such a lethal reciprocal translocation of genetic material. Chronic myelogenous leukaemia (CML) results from translocations of DNA of chromosomes 9 and 22 and the formation of an abnormally short chromosome 22, known as the Philadelphia chromosome, and a leukaemia-inducing protein. The introduction of imatinib, an inhibitor of this pathogenic protein, has revolutionised its management – just as the use of arsenic to combat APL did.
Prompt diagnosis and effective treatment
APL is potentially so rapidly lethal that experts recommend that patients suspected with this form of leukaemia be treated immediately, without waiting for molecular diagnostic confirmation. In fact, since a single abnormal fusion gene encoding a specific new protein is involved, there should be little difficulty in developing new, rapid genomic or immunodiagnostic assays. Unfortunately, as APL is such a rare form of leukaemia the economic incentives for drug companies and private healthcare services to develop such tests may not be compelling.
APL has been described as the first malignant disease highly curable with targeted therapy directed at a unique molecular abnormality. However, despite the dazzling response rates seen in clinical trials for ATO-ATRA combinations, APL patient registries show that early deaths are still common in ‘real-world’ clinical practice. This may partly be attributed to delayed diagnosis and treatment. It is also possible that some APL patients in clinical practice differ from those recruited to trials, notably in age and risk categories. Nonetheless, there is ongoing work aimed at identifying possible predictors of non-response to ATO-ATRA.
An oral ATO alternative to the present injectable form should make this drug more widely accessible, if early evidence of equal efficacy of the two dosage forms is confirmed by ongoing trials.
It is an irony that as the efficacy of the two novel APL drugs have become more widely recognised, their prices, low in China, have ballooned in the West. Perhaps Conan Doyle’s Sherlock Holmes and Agatha Christie’s Miss Marple should be sent to investigate this case of what economists refer to as market inefficiency. As with the ATO-ATRA combination, their joint efforts should be synergistic – producing a greater combined effect than the sum of their individual effects.
Professor Alain Li Wan Po is editor-in-chief of the Journal of Clinical Pharmacy and Therapeutics, and is a fellow of the Royal Pharmaceutical Society and the Royal Statistical Society.
–