Definition
The use of genetic and genomic information to tailor pharmaceutical treatment to an individual.
Use in clinical context
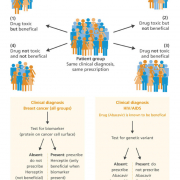
Pharmacogenomics combines pharmacology – the science of drugs – with genomics – the study of the genome and its functions. Its aim is to use information about a person’s genomic make-up to identify the most effective drug for them, to minimise side effects and find the ideal dosage.
There are two aspects of drug function that can be affected by DNA variation in an individual’s genome. The first is known as pharmacokinetics – that is, how the drug is distributed, metabolised and excreted by the body. Some drugs also need to be broken down by the body for them to be active, and the body’s ability to break down a particular drug can be markedly influenced by DNA variation. The second aspect is pharmacodynamics, which is the effect a drug has on its target in the body – a major factor in efficacy. Pharmacodynamics also encompasses ‘off-target’ effects of drugs – a major factor in side effects.
A classic example of pharmacogenomics in current practice is the antiretroviral drug Abacavir, used in the treatment of HIV/AIDS. About 5% of people will have a severe hypersensitivity reaction to this drug, which in some cases is life threatening. These individuals have a specific DNA variant of the HLA-B gene, HLA-B5701. This gene encodes for a protein that plays a critical role in the immune system. Testing for this allele is required before Abacavir is prescribed in the UK and has dramatically reduced the occurrence of this hypersensitivity reaction.
Related terms
Deoxyribonucleic acid (DNA) | Gene | Genomics | Off-target effects | Protein | Variant