Newborn blood spot screening
Newborn blood spot screening is offered to parents to test babies for 10 rare but serious health conditions. Early diagnosis and treatment can improve the health of affected individuals and may prevent complications, including severe disability and death.
Overview
Newborn blood spot (NBS) screening is undertaken via a heel prick test, optimally around day five after birth. Results are typically available within six weeks.
Conditions
The NBS screening programme enables early identification, referral and treatment of babies with any of the following conditions:
- cystic fibrosis (CF);
- congenital hypothyroidism (CHT);
- glutaric aciduria type 1;
- hereditary tyrosinemia type 1;
- homocystinuria;
- isovaleric acidaemia;
- maple syrup urine disease;
- medium-chain acyl-CoA dehydrogenase deficiency (MCADD);
- phenylketonuria; and
- sickle cell disease (SCD).
A pilot evaluation has been undertaken in some areas of England to screen specifically for severe combined immunodeficiency, a group of rare genetic conditions that affect the development and function of the immune system and cause a newborn to be susceptible to infections. Final data analysis is currently underway, with recommendations to follow.
Inheritance patterns
Most of the conditions being tested for during NBS screening are inherited in an autosomal recessive pattern (see figure 1).
Figure 1: Autosomal recessive inheritance
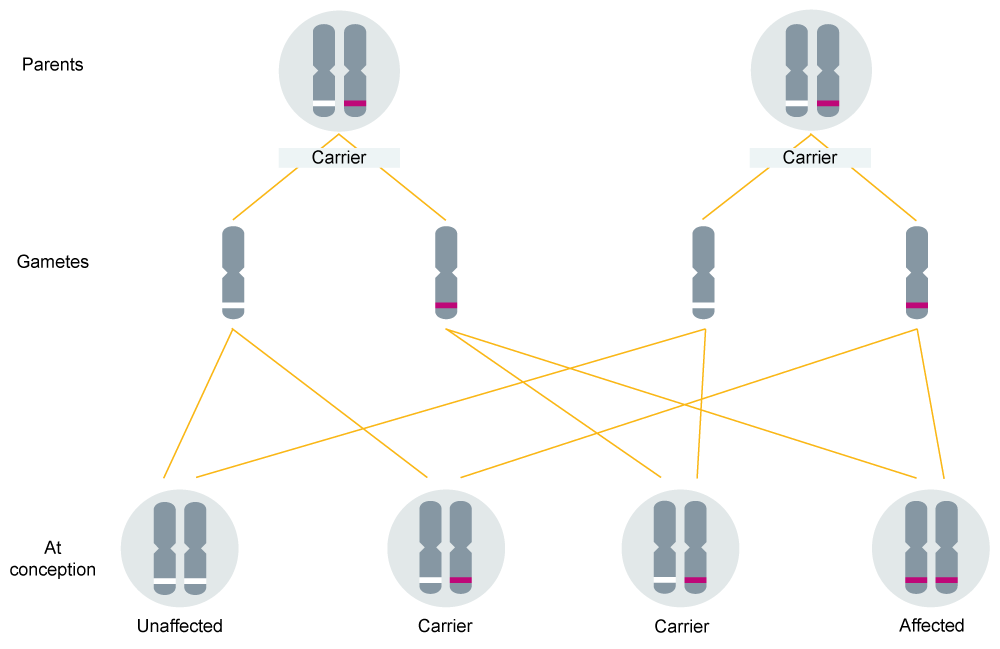
This means that any findings may have implications for other family members. Patients can speak to their midwife or GP about this and, if required, can be referred to a genomic counsellor for further support and testing.
Counselling patients
It is the health professional’s responsibility to explain NBS screening to parents and to offer it for their baby.
This conversation should be initiated during the antenatal period. It is recommended that couples are asked if there is a family history of any of the 10 conditions; if history is identified, a care plan can be put in place prior to the birth. Providing this information during the antenatal period also allows parents appropriate time to consider their options and ask questions.
The health professional should provide parents with the guidance document ‘Screening tests for you and your baby‘, which is available in 13 languages.
Parents are asked for verbal consent for NBS screening. They can opt out of testing for SCD, CF and CHT individually, but testing for the seven inherited metabolic diseases is completed as a group.
Babies who are premature or are admitted to a neonatal unit will have additional recommendations for screening.
Taking the sample
NBS screening is a blood sample taken from the child’s heel (see figure 2).
Figure 2: Taking the blood sample for NBS screening

Image taken from NHS Health A to Z: Newborn blood spot screening FAQs. Licensed under the Open Government License v3.0.
The optimum time for testing is on day five following birth; however, children are eligible for screening up until their first birthday for every condition except CF, for which the test is no longer reliable after eight weeks of age. Samples should be sent to the screening laboratory for analysis on the same day that they are taken.
For further information about NBS sampling, please read through the sampling guidelines., You can also access guidance on how to take a good-quality sample.
Results
Parents usually receive the results of the NBS test within six weeks. If a condition is suspected, the parents will be contacted as soon as possible so that the child can have further testing or treatment immediately. The results must be given by an appropriately-trained and knowledgeable clinician, and parents should be provided with the national guidance about screening for the 10 conditions (see the resources for patients below).
Key messages
- Newborn blood spot (NBS) screening is offered to parents to test their baby for 10 rare but serious health conditions for which early diagnosis and treatment can improve the baby’s health.
- NBS screening is undertaken via a heel prick blood sample, ideally around day five following birth.
- Parents usually receive the results of the NBS test within six weeks.
Resources
For clinicians
- Great Ormond Street Hospital for Children NHS Foundation Trust: Severe combined immunodeficiency (SCID)
- Gov.uk: Final data analysis underway to inform SCID screening recommendation
- Gov.uk: Newborn blood spot sampling guidelines: quick reference guide
- Gov.uk: Newborn blood spot screening: programme handbook
- Gov.uk: Newborn blood spot screening standards valid for data collected from April 2021
- Gov.uk: New resources to help improve quality of samples taken in NHS newborn blood spot screening
- NHS Newborn Blood Spot Screening Programme: Community midwife discusses how she reduced her avoidable repeat rate (video, three minutes 12 seconds)
- NHS Newborn Blood Spot Screening Programme: Online course collection
- St George’s University of London: Genetic inheritance for the pregnancy pathway: A practical guide for clinicians
For patients
- Gov.uk: Screening tests for you and your baby
- NHS: Blood spot tests: An easy guide to screening tests for your new baby (PDF, 12 pages)
- NHS: Newborn blood spot test